By Sarah Kliff
Washington Post, April 26, 2013
Welcome to Health Reform Watch, Sarah Kliff’s regular look at how the Affordable Care Act is changing the American health-care system — and being changed by it. You can reach Sarah with questions, comments and suggestions here. Check back every Monday, Wednesday and Friday afternoon for the latest edition, and read previous columns here.
There’s pretty widespread agreement, on both sides of the aisle, that the health-care law will expand insurance coverage. The nonpartisan Congressional Budget Office estimates that 30 million more Americans will have health insurance by the end of a decade.
What’s become more of a debate though, is how good that health insurance coverage will be. Two new academic studies raise the possibility that many Americans will still face big financial burdens after they gain insurance coverage.
“The Affordable Care Act will reduce the number of uninsured by a little more than half, which is a good thing,” says Stephanie Woolhandler, a professor at the CUNY School of Public Health. “But it’s going to increase the problem of underinsurance: People who have insurance but still can’t afford care.”
The whole point of buying health insurance coverage is to make care affordable. Millions of Americans pay monthly premiums with the expectation that, should a horrible illness or accident occur, the insurance company will cover the majority of some pretty expensive hospital bills.
Some experts and health advocates have begun to question whether the health-care law can deliver on that promise. Woolhandler wrote an editorial earlier this week, in the Journal of General Internal Medicine, contending that “the new private coverage offered to the near-poor and middle income individuals through insurance exchanges will also leave many underinsured.”
Much of this has to do with the type of plans that insurers will sell on the health insurance exchange. Health insurers will offer consumers a “bronze” plan that will, on average, cover 60 percent of an enrollee’s costs. This, in health insurance-speak, is known as “actuarial value.” Using actuarial values can make it easier to compare plans, and understand what part of the bill the insurer will likely cover — and how much the enrollee can expect to be on the hook to pay.
The exchange will also have other plans with different actuarial values: Silver plans will cover 70 percent of an average enrollee’s costs, and gold plans would be expected to foot 80 percent of the bill. The bronze plans are expected to attract a high number of enrollees, since they will likely have smaller premiums — because consumers are buying less robust financial coverage.
Woolhandler, who is the co-founder of Physicians for a National Health Program, has previously conducted research on rates of medical bankruptcy in Massachusetts, before and after the state expanded health insurance access. She found that in 2009, two years after the insurance expansion took effect, just about half the debtors (52 percent) attributed their bankruptcy at least in part to medical bills. In 2007, before the expansion, the number stood at 59 percent.
Allison Gailbrath, an assistant professor at Harvard Medical School, has also looked at the Massachusetts’s insurance expansion to better understand how access to health insurance affects the financial burden of medical costs.
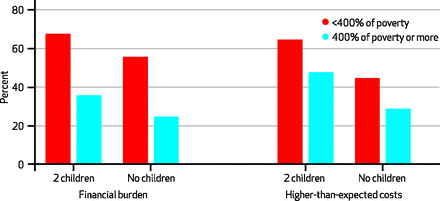
She published a paper this month in the journal Health Affairs, which looked at which costs were faced by families who had gained insurance through the Connector, Massachusetts’s version of a health-care exchange. She found that 38 percent reported a financial burden (defined as having difficulty paying medical bills) and 45 percent said costs were higher than they had expected.
Numbers were slightly higher for those earning less than 400 percent of the poverty line and for those with children.
It’s worth noting that the Massachusetts bronze plans had a lower actuarial value than those that will be sold on the exchanges. They covered, on average, 40 to 50 percent of enrollees’ costs. That means, to Gailbraith, that underinsurance is still a concern in the federal exchanges—but perhaps not as much as it has been in the Massachusetts experience.
“The exchanges will provide coverage and that will help the uninsured but there’s still an underinsured problem,” Galbraith says. “People will have plans, but they will still have cost issues involved.”
Galbraith contends that this creates an impetus for better consumer education — that there’s space for better education about how much health insurance will cover, and what consumers might be expected to pay. Some employers, for example, will provide cost calculators where enrollees can input some data on what type of health-care spending they expect and get a sense of which plan might provide the best deal.
That can move consumers away from just comparing premiums, and towards thinking about all the other costs they could incur from various co-payments and cost-sharing. That could lead consumers to pick different plans, which might come with higher premiums — but also lower cost-sharing down the line.
KLIFF NOTES: Top health policy reads from around the Web.
Senate Democrats are concerned about Obamacare’s roll out. “Democrats in both houses of Congress said some members of their party were getting nervous that they could pay a political price if the rollout of the law was messy or if premiums went up significantly. President Obama’s new chief of staff, Denis R. McDonough, fielded questions on the issue for more than an hour at a lunch with Democratic senators.” Robert Pear in The New York Times.
As time runs out, Florida’s Medicaid expansion hangs in limbo. “House Republicans rejected a bipartisan Senate proposal to accept $51 billion in federal health care money on Thursday, diminishing hopes that lawmakers will reach a health care compromise before the legislative session ends next week.” Tia Mitchell in the Miami Herald.
Mid-level health care jobs are disappearing. ”Positions such as licensed practical nurses and medical-records clerks are being eliminated or pushed out of hospitals into lower-paying corners of the field such as nursing homes. Meanwhile, positions that were once an accessible first rung on the career ladder, such as registered nursing, increasingly require at least a bachelor’s degree.” Ben Casselman in The Wall Street Journal.
Correction: This story originally misstated the actuarial value of the bronze plans in the Massachusetts Connector. It is between 40 to 50 percent.
http://www.washingtonpost.com/blogs/wonkblog/wp/2013/04/26/will-obamacare-end-medical-bankruptcies-probably-not/
