By Ahmed Kutty, M.D.
Granite State Chapter PNHP, Sept. 14, 2016
The following text is an unofficial, lightly edited transcript of testimony delivered by Dr. Ahmed Kutty to a subcommittee of New Hampshire’s House Health, Human Services and Elderly Affairs Committee on Sept. 14, 2016. The session was co-chaired by state Reps. Thomas Sherman, M.D., and John Fothergill, M.D.; and included subcommittee member Rep. Susan Emerson.
1. The Affordable Care Act is not enough. The ACA, now in its third year of implementation, has failed to provide universal, affordable access to care and to control costs. Forty-three percent of enrollees in the ACA report the plan costs to be unaffordable (Commonwealth Fund study). For the impact (in numbers) of the ACA and under our current system, on the uninsured, underinsured, on medical bankruptcy and on preventable (nonviolent) deaths, see table below:
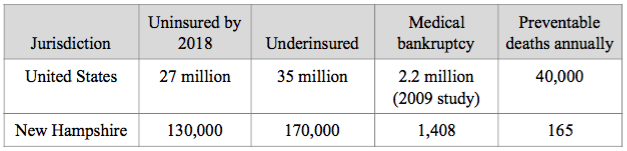
Complexity and opaqueness are built into the private system, in contrast to the simplicity and transparency of a public system.
2. U.S. expenditure on health care is twice the average of other advanced economies per capita, and as a percent of GDP. See graph below:
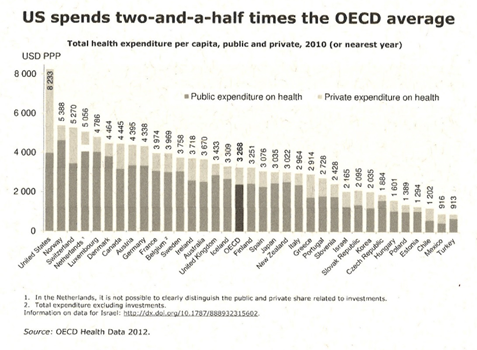
3. Economic benefits. Health care expenses borne by business do not enhance value and add to the cost of goods and services, passed on to the consumer. Removing the cost burden of employee health insurance from businesses, large, medium and small, could increase the profit margin and potentially lead to job growth via reinvestment in expansion and innovation, thus facilitating rejuvenation of the local and regional economy.
Workers aged 50 to 64 are often expensive to insure and less likely to find new employment opportunities. Delinking health insurance and employment will increase work-related mobility in this demographic segment. Job loss from illness will not result in loss of coverage, frequently when most needed, as under the current system.
A public system will remove an onerous obligation currently heaped on local entities such as municipalities, school boards and county governments.
4. Cost control by means of price negotiations for drugs, durable equipment, devices, hospital stays and fees for professional services are integral to a publicly funded system. Nationally, savings of $650 billion annually is projected from these measures and from reduction of wasteful administrative spending that prevails in our current, fragmented, multi-payer system, with about 6,000 plans operating in the country, offering 28,000 “products”! This is money siphoned off from funding for direct patient care in all settings.
5. Societal health. The U.S. ranks 19th in the world, in measures of population health as life expectancy, infant mortality and other preventable causes of death, mostly due to lack of access to affordable and timely health care.
6. Administrative advantages. Medicare overhead is 3 percent vs. private insurers’ average of 18 percent – and in some plans up to 28 percent – generated by the need to advertise, distribute dividends to shareholders, and pay exorbitant CEO salaries.
7. Single Payer vs. Socialized Medicine. Single payer is system of privately delivered and publicly funded care, like our Medicare and the Canadian Medicare. The Veterans Health Administration, the military medical system, the Indian Health Service, and the National Health Service in UK are examples of “socialized” systems.
8. Electronic medical records (EMR). A streamlined, interoperable, nationwide information system, similar to the VISTA in use by the Veterans Administration for over a decade, will help reduce waste and redundancy and improve efficiency, if it is designed with clinical utility and service benefit, rather than the bottom line of the vendors, as the focus. At the state level, such a system will be organic to a publicly funded program.
9. Physicians’ and public support. New Hampshire doctors supported a “simplified payer system with public funds” by a two-third majority in a study by the NH Medical
Society in 2007. In several surveys, a tax-funded financing system has enjoyed public support at 60 percent to 70 percent level nationally, over the last two decades.
10. Public health issues. A publicly funded system is significantly better designed to deal with epidemics like opioid addiction (prevention, treatment and rehabilitation), a major public health crisis in our state and in the New England region.
11. Activity in other states. California, New York, Vermont, Oregon, Hawaii and others have bills to legislate or for study commissions to get “a single pipeline mechanism” established for public funding of ALL medically necessary, comprehensive health care services, including drugs and devices. Colorado has a ballot initiative (Amendment 69), with enormous potential to engender systemic change, if it is approved by voters this November.
Therefore a Study Commission to consider all aspects of a “Medicare for All” system, providing universal, medically appropriate care through public funding, is strongly warranted and eminently worthy of bipartisan support in the General Court.
As members of the Granite State chapter of the Physicians for a National Health Program, we request your careful consideration of the above bullet points and to take action leading us towards creation of a health care system that supplies truly universal, affordable, high-quality comprehensive care, in a fiscally sustainable milieu here in New Hampshire. Your public voice and your vote for the Study Commission bill will be a major contribution to the sustained multipronged effort needed for resolving the looming crisis in health care facing our state and very likely for the nation as well.
Thank you, Dr. Sherman, for giving me the opportunity to speak before your esteemed subcommittee today on this critical issue that has been concerning our society for over a century. Having heard us, can we hope our words will be heeded?
Ahmed C. Kutty, M.D., FACC
Peterborough, NH
